Risky Business forum probes learnings from the pandemic, ways forward

Risky Business full program, April 15, 2021
A unique patient safety conference, hosted virtually last week by a group of Boston-based health care organizations including the Betsy Lehman Center, featured a series of rapid-fire presentations and conversations about managing through — and emerging stronger from — the COVID-19 pandemic.
One key theme was the exposure of long-standing, deep racial inequities in our country, including in health care.
“One of the key takeaway lessons of the COVID era is that we are, I hope, finally recognizing how horrific the heritage of inequity is in this country,” said Donald M. Berwick, M.D.,
President Emeritus at the Institute for Healthcare Improvement.
Liz Miranda, "When COVID hits home: My family, my community"
Massachusetts State Representative Liz Miranda said that if our collective COVID experience provides any glimmer of hope, it lies in a renewed awareness and greater public recognition of racial inequity and injustice. Miranda represents the 5th Suffolk, the Commonwealth’s most diverse legislative district, which was disproportionately affected by COVID-19. Speaking on behalf of her constituents, as well as her extended Cape Verdean-American family, Miranda said, “There should be no going back to ‘normal’ because normal was never good enough.”
The virtual conference was the most recent Risky Business event in a series built on the premise that health care can learn from high-risk industries and other endeavors that confront similar safety challenges and was a collaboration of the Betsy Lehman Center, Boston Children’s Hospital, and CRICO: The Risk Management Foundation of the Harvard Medical Institutions, in partnership with Dana Farber Cancer Institute, Institute for Healthcare Improvement, Massachusetts General Hospital, Massachusetts Health & Hospital Association, and Massachusetts Medical Society.
Peter Laussen, M.B.B.S., Executive Vice President of Health Affairs at Boston Children's Hospital and Professor of Anesthesia at Harvard Medical School, is a Risky Business co-founder. He joined Barbara Fain, Executive Director of the Betsy Lehman Center for Patient Safety, in hosting the live event from Boston. Nearly 1,500 participants joined the forum, which was moderated by Boston Globe reporter Robert Weisman and WBUR’s Martha Bebinger.
With experience in organizations as varied as the U.S. Army, the National Football League and hospitals in Boston and Toronto, other speakers described ways to manage the pressures and uncertainty COVID-19 has imposed on all sectors of health care.

Kevin Churchwell, Introductory remarks
The forum began with introductory remarks from Kevin Churchwell, M.D., President and CEO of Boston Children’s Hospital, said the pandemic forced him and other leaders to think in terms of piloting a speedboat versus the ocean liner that hospitals typically resemble. Churchwell found that the pandemic posed challenges different from those anticipated by “normal” crisis management planning and noted that coordinating with other hospital CEOs and leaders from the state’s COVID-19 Command Center was key to managing the crisis.
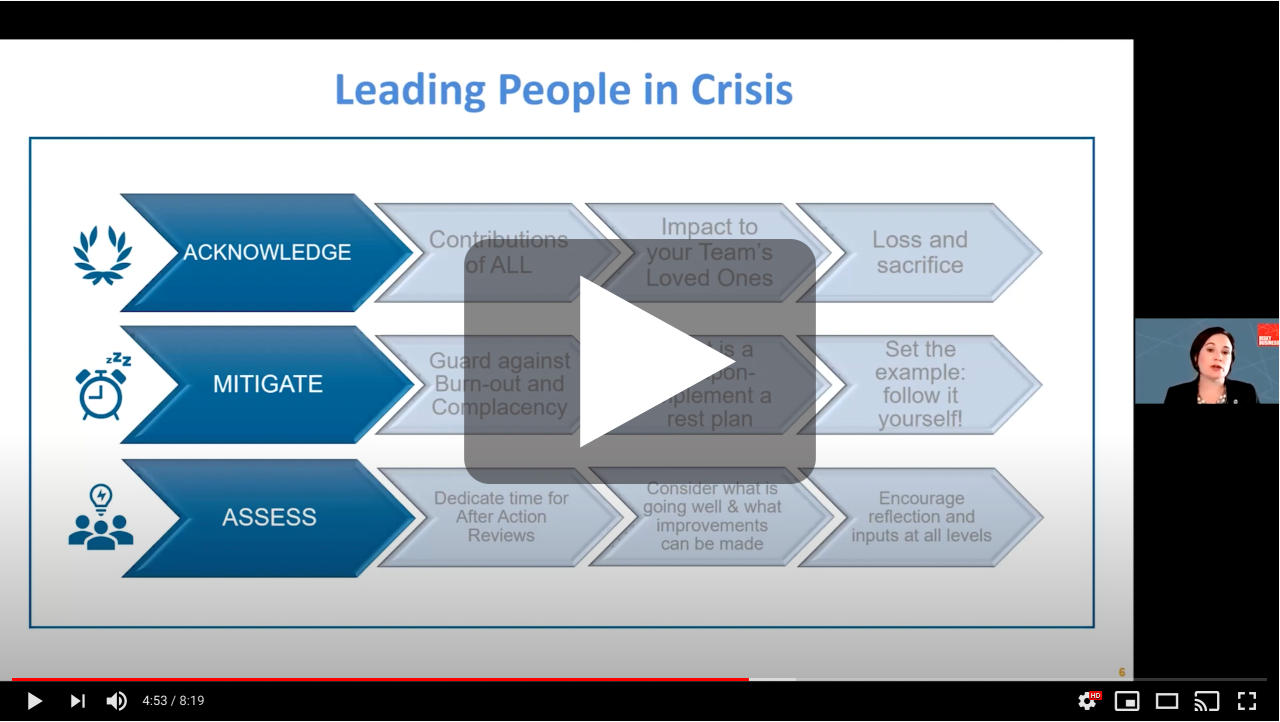
Sue Gannon, "Leadership in a prolonged crisis"
Lieutenant Colonel Susan M. Gannon, who served with the U.S. Army in Afghanistan, agreed that COVID-19 presented a new kind of crisis. Unlike the mass casualty events that hospitals typically train for, the pandemic touched every aspect of operations and all staff. Gannon, who worked with Tufts Medical Center and Tufts University to manage the COVID crisis early in the pandemic, talked about balancing the needs of patients, employees, the enterprise and the public. Her best approach is to “focus on decision-making and the people you serve” with efficiency and transparency.
Patricia Trbovich, "Underscoring the 'human' in human factors"
Patricia Trbovich, Ph.D., Research Chair in Patient Safety and Quality Improvement at North York General Hospital in Toronto, Ontario, urged leaders to concentrate on positioning their employees for success. Especially under the pressure of COVID-19, leaders must understand that individuals react in their own way in high-risk situations and need to be able to calibrate their actions to immediate circumstances. Maintaining team effectiveness and cohesion in high-stress, fluid circumstances requires good information, leadership skills and dexterity. “Know your people,” said Dr. Trbovich, “and how to unite them.”

Josh McDaniels, "The public is watching: A look inside the NFL during COVID-19"
As Offensive Coordinator and Quarterback Coach for the New England Patriots, Josh McDaniels relied on leadership skills and strategies he usually applies to football to help guide the team safely through the season. Similar to hospitals and other organizations, the Patriots used cloud-based applications for training and safety information. Navigating the season also involved constant testing for COVID-19, the use of personal tracking technology and quickly adjusting to changing circumstances. The team also hosted virtual social events for team members and their families. McDaniels emphasized that it was challenging but, in the end, successful. Having been on the coaching staff for the Patriots’ six Super Bowl-winning teams, McDaniels said, “Our teamwork has never been better” than it was during the pandemic.
Karthik Sivashanker, "Advancing racial justice and equity through quality and safety: 5 key drivers"
Karthik Sivashanker, M.D., Medical Director for Quality, Safety and Equity at Brigham and Women’s Hospital and Vice President of Equitable Health Systems and Innovation at the American Medical Association, focused his remarks on racial justice and challenged safety and quality professionals to make it part of their mission. He observed that the disparities revealed and exacerbated by COVID-19 serve as “a stark reminder of the peril of disconnecting our work from the core principles of morality, equity and justice … We are not delivering high quality care if it’s only for a small portion of the population.”
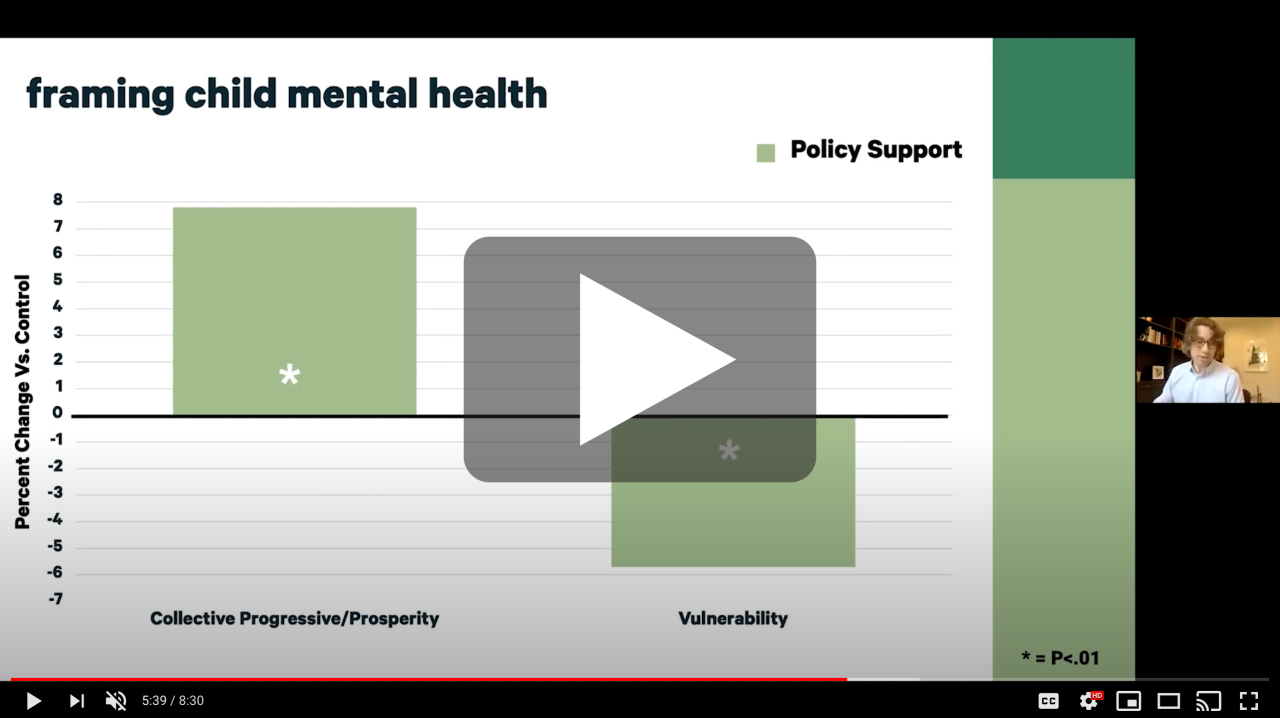
Nat Kendall-Taylor, "Time for change: Framing to move minds"
Nat Kendall-Taylor, Ph.D., noted that COVID-19 has forced many people to question their fundamental understanding of how the world works. Dr. Kendall-Taylor is CEO of Frameworks Institute, a non-profit research firm that studies the public's understanding of important social issues and how best to frame those issues for effective communication. He described the value of using explanatory language to talk about complex topics, including patient safety and inequities in health care. “There needs to be a lot more explanation about how systems have been set up historically to favor certain groups. The answer is not a one sentence slew of magic words that will suddenly create ah-ha moments about structural racism,” Kendall-Taylor said.